It's a New Day in Public Health.
The Florida Department of Health works to protect, promote, and improve the health of all people in Florida through integrated state, county, and community efforts.
Chagas Disease

It is estimated that as many as 8 to 11 million people in Mexico, Central America, and South America have Chagas disease. Most people are asymptomatic and do not know they are infected. However, approximately 20 to 30 percent of those with chronic infection will develop clinically apparent disease, making it a significant public health concern.
- Symptoms and Treatment
- Transmission
- Blood Screening for Chagas Disease
- Resources
Symptoms
Once transmission has taken place, most infected individuals experience an acute illness phase with mild symptoms or nonspecific febrile illness that frequently goes unrecognized. After four to eight weeks or more, individuals enter the chronic phase and parasites are generally not detected in the blood. Without treatment, they will remain infected for life. As previously mentioned, some people will remain asymptomatic (indeterminate infection) but others (20-30%) will experience clinical symptoms including cardiac damage. This can range from mild changes on electrocardiogram to severe arrhythmias, cardiomyopathy, and sudden death. The digestive tract can also be involved leading to megaesophagus or megacolon. Finally, the peripheral and central nervous systems can be affected.
Treatment
Infected individuals should be referred to a local physician or clinic for follow-up care and treatment. In the United States, antitrypanosomal medication (nifurtimox or benznidazole) is only available through CDC. The physician should call CDC to determine whether treatment is indicated. The CDC consult line for physicians is 404-718-4745. Medications are free of charge for eligible patients and will be shipped directly to the physician’s office.
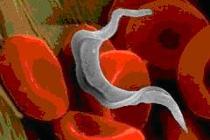 Chagas disease is caused by infection with Trypanosoma cruzi, a protozoan parasite. In Chagas endemic countries, it is typically transmitted by infected triatomine bugs (commonly known as kissing bugs). The insects defecate during or after feeding and the feces enter the human body through the bite wound or mucous membranes. Alternatively, transmission can occur congenitally (from mother to fetus), through blood transfusion or organ transplantation, accidental laboratory exposure, or rarely through ingestion of food contaminated by infected bugs. Transmission in the United States is rare and does not follow the same pattern as endemic countries. Congenital and transfusion transmission are more common, mostly attributed to better housing conditions. Additionally, the triatomine species present in the United States (Triatoma sanguisuga) prefer animal hosts.
Chagas disease is caused by infection with Trypanosoma cruzi, a protozoan parasite. In Chagas endemic countries, it is typically transmitted by infected triatomine bugs (commonly known as kissing bugs). The insects defecate during or after feeding and the feces enter the human body through the bite wound or mucous membranes. Alternatively, transmission can occur congenitally (from mother to fetus), through blood transfusion or organ transplantation, accidental laboratory exposure, or rarely through ingestion of food contaminated by infected bugs. Transmission in the United States is rare and does not follow the same pattern as endemic countries. Congenital and transfusion transmission are more common, mostly attributed to better housing conditions. Additionally, the triatomine species present in the United States (Triatoma sanguisuga) prefer animal hosts.
Infected triatomine bugs and infected reservoirs, such as raccoons, have been identified in Florida. However, the risk of local transmission to people in Florida is low. There have been cases of local transmission in Texas, Tennessee, California, and Louisiana. People in less affluent areas of Florida likely have a greater chance of becoming infected.
Since the introduction of blood donation screening for Chagas in 2007, more chronic infections in the United States are being recognized. The blood centers perform an enzyme-linked immunosorbent assay (ELISA). Donations that have repeat reactive ELISA should be confirmed with a radioimmuno-precipitation assay (RIPA). In a 2005 study by the American Red Cross to evaluate the Chagas screening assay used by blood donation centers, 51% of donors with repeat reactive screening tests had positive results on RIPA. Due to the cost of RIPA, some blood centers opt not to perform confirmatory testing since the blood is not used if ELISA is positive. Blood centers to perform RIPA as a public health service. Blood banks should notify individuals with positive results and ideally both provide contact information for the county health department to the donor and notify the CHD of the result. CHDs are encouraged to develop relationships with blood centers to facilitate this flow of information.
Additional information on Chagas disease can be found at the Centers for Disease Control and Prevention (CDC).
*Note: This page contains materials in the Portable Document Format (PDF). The free Acrobat Reader may be required to view these files.



Connect with DOH