It's a New Day in Public Health.
The Florida Department of Health works to protect, promote, and improve the health of all people in Florida through integrated state, county, and community efforts.
Plague

Plague is an acute, bacterial disease caused by Yersinia pestis, a Gram-negative bacteria that is transmitted from rodent to rodent by infected fleas.
- SYMPTOMS AND TREATMENT
- TRANSMISSION
- PLAGUE OCCURRENCE IN FLORIDA
- REFERENCES
Signs and symptoms include fever, headache, myalgia (muscle aches), malaise, shaking chills, prostration, and gastrointestinal symptoms. Several antibiotics may be used for prophylactic therapy in persons exposed to Y. pestis, although streptomycin is the drug of choice. An inactivated vaccine is also available in the United States.
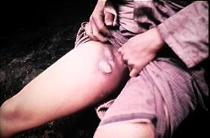
The three principal clinical presentations of plague are bubonic, septicemic, and pneumonic. Bubonic is the most common, with an incubation period from 2-6 days, and is characterized by the development of an acute regional lymphadenopathy (swollen lymph nodes), or bubo. The case-fatality rate for untreated individuals is 50-60%. A septicemic form of the disease occurs when Y. pestis invades and multiplies in the bloodstream. This can occur secondarily to the bubonic form or develop without detectable lymphadenopathy. Pneumonic plague is the least common, but most fatal, form of the disease. It can develop either as a secondary complication of septicemia or result from inhalation of infectious respiratory droplets expelled from a human or animal that has the pneumonic form. The incubation period for primary pneumonic plague is 1-3 days.

The most common mode of transmission Y. pestis to humans is by the bite of infectious fleas, especially the Oriental rat flea (X. cheopis). Less frequently, infection is caused by direct contact with infectious body fluids or tissues while handling an infected animal or inhaling infectious respiratory droplets.
Outbreaks of plague in humans usually involve exposure to house rats and their fleas. Risk for plague in humans is greatest when epizootics cause high mortality in rat populations, thereby forcing hungry, infected rat fleas to seek alternative hosts such as humans. The last rat-borne epidemic in the United States occurred in Los Angeles in 1924-25. Since then, all human plague cases in the U.S. have been sporadic cases acquired from wild rodents or their fleas or from direct contact with plague-infected animals. Rock squirrels, ground squirrels, prairie dogs, wood rats, and chipmunks have served as sources of human infection. Domestic cats have recently been sources of infection for humans.
The last reported case of human plague in Florida occurred in 1920 during an outbreak in Pensacola. The disease still remains a threat, however, because of enzootic foci in the wild rodent populations of several western states. Even though plague is not currently in Florida, there is always the possibility that animals infected with Y. pestis may be imported into areas of the state that have suitable flea vectors (including Xenopsylla cheopis).
Bigler WJ and Janowski DD. Bubonic plague in Florida??! Epi Update (Florida Department of Health, Bureau of Epidemiology).
Benenson AS (ed.). Control of Communicable Diseases Manual, Sixteenth Edition. United Book Press, Baltimore. 1995: 353-358.
Layne JN. Fleas (Siphonaptera) of Florida. Florida Entomologist. 1971; 54(1):35-51. March 6,1997:1-2.
CDC. Prevention of Plague: Recommendations of the Advisory Committee on Immunization Practices (ACIP). Morbidity and Mortality Weekly Report. December 13, 1996;45 (no. RR-14).
CDC. Information on Plague. Internet address (accessed September 2005): https://www.cdc.gov/plague/
CDC. Human plague; United States, 1993-1994. Morbidity and Mortality Weekly Report. April 8, 1994; 43(13):242-246.
CDC. Fatal human plague; Arizona and Colorado, 1996. Morbidity and Mortality Weekly Report. July 11, 1997; 46(27):617-620.



Connect with DOH