It's a New Day in Public Health.
The Florida Department of Health works to protect, promote, and improve the health of all people in Florida through integrated state, county, and community efforts.
Varicella (Chickenpox) in Florida
Florida Health
Disease Control- DiseaseControl@flhealth.gov
- 850-245-4444
-
Florida Health
4052 Bald Cypress Way
Tallahassee, FL 32399
April Key Points
outbreaks
highest incidence
up-to-date or
unknown vaccinations status
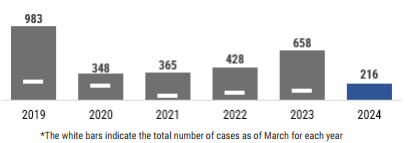
The number of varicella cases reported in April 2025 increased from the previous month and was above the previous 5-year average. Due to robust vaccination programs, there is no longer discernable seasonality for varicella cases in the United States.
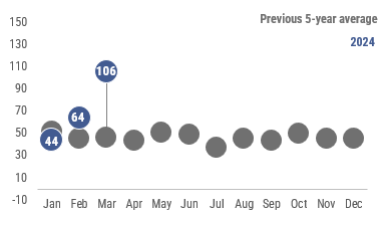
In April 2025, 58 varicella cases were reported in 21 counties, outlined in black in the map. From February 2025 through April 2025 the average county rates varied throughout the state.
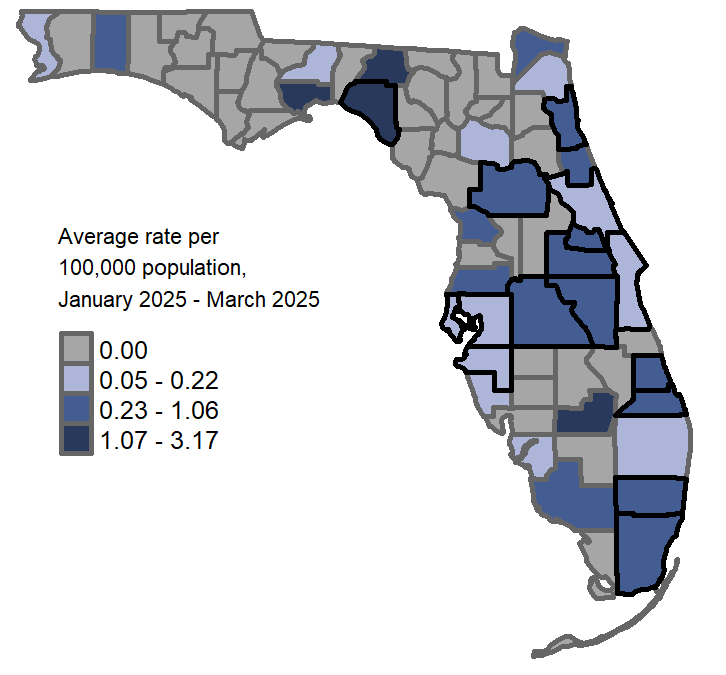
In 2025, 189 varicella cases were reported. The annual number of reported varicella cases gradually increased from 2020 to 2024.
*CDC MMWR report year
In April 2025, the varicella rate was highest among <1-5 year olds at 1.44 cases per 100,000 population. Infants <1 year old are too young to receive varicella vaccination, which is why vaccination of siblings, parents, grandparents, and other age groups is important in infection prevention among infants.
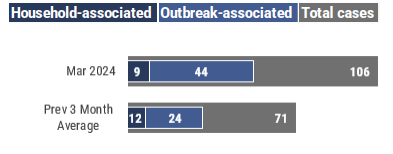
In April, 13 cases were household-associated and 1 case was outbreak-associated. For most varicella cases, exposure to other known cases is not identied. In Florida, transmission setting is not routinely identied for non-outbreak cases.
People with shingles infection can transmit the virus that causes varicella to people without immunity. In April, 11 cases reported having contact with someone diagnosed with shingles during their exposure period. In April 2025, 33% of cases reported with varicella had not received the recommended number of varicella vaccinations for their age or had unknown vaccination status. Vaccination against varicella is important for infants, children, teenagers, and adults. If a person was born before July 1, 1994, the current varicella immunization recommendation would not have been implemented when they were receiving their childhood immunizations. Based on the case’s age, 52 cases in 2025 would not have been vaccinated under the current childhood immunization recommendations.
In 2025, the majority of adults aged 19 years and older with varicella were not up-to-date on their varicella vaccinations or had unknown vaccination status. Although individuals who have been vaccinated can still develop varicella, complete and timely vaccination remains the best way to prevent varicella and severe complications.
*Note: This page contains materials in the Portable Document Format (PDF). The free Acrobat Reader may be required to view these files.



Connect with DOH